Attendees at the Conference will hear from a broad range of speakers on several streams of concurrent scientific and non-scientific sessions, with engaging invited speakers, interactive workshops and social functions to suit everyone.






































This workshop will empower participants to share stories of exceptional self, peer and patient care, as well as participate in a number of simulated experiences aimed at reconnecting them with the vulnerability experienced by their patients. The concepts of self-care and care for teammates will also be addressed.
Learning outcomes:
*This is a Member Benefit, available only to members of an affiliate professional body.
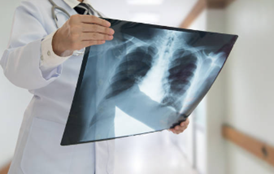
This interactive workshop will develop fundamental image interpretation knowledge and skills for conventional chest X-rays. Using a systematic approach, participants will practise interpreting anonymised clinical cases and write preliminary image evaluations to communicate urgent and unexpected findings. Pathologies explored will include commonly present acute chest conditions, thoracic trauma, pleural and mediastinal abnormalities, iatrogenic devices and acute abdominal abnormalities demonstrated on chest X-ray.
Learning outcomes:
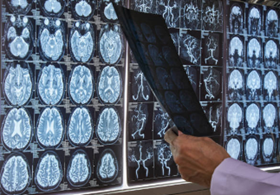
Join renowned Dr Charbel Saade for this informative and highly engaging workshop. Gain knowledge of the patterns and mechanisms of gadolinium enhancement to facilitate radiologic differential brain diagnosis and the blood-brain barrier. Understanding the classic patterns of lesion enhancement—and the radiologic-pathologic mechanisms that produce them—can improve image assessment and differential diagnosis. This workshop will cover cross-sectional anatomy and pathology.
Learning outcomes:
Effective clinical supervision and training of students is sometimes challenging to deliver in fast-paced medical imaging and radiation therapy departments, but it is essential for developing the future workforce. This interactive workshop, delivered by experienced clinical educators, aims to equip staff with practical knowledge and techniques for supporting, encouraging and training students with minimal resource requirements and impact on service delivery.
Learning outcomes:
Getting started in research can be challenging when you are not sure where to begin. The aim of this workshop is to provide practical support for those who have a research idea they wish to develop or those who would like to become involved in research and want to know where to start. Strategies for getting started in research will be presented followed by small group work developing existing research ideas or working through prepared examples.
Learning outcomes:
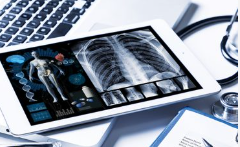
This workshop will provide participants with knowledge of current and future uses of AI in medical imaging and radiation therapy, how it may impact the medical radiation practitioner roles, ethics, education, and the opportunities that it presents to medical radiation professions.
Learning outcomes:
This workshop will cover:
Learning outcomes:
Getting a paper published is easier than you think. Join this workshop and learn practical tips to successfully publish in a peer reviewed journal. Share your experience and ask questions to a panel of editors, reviewers and authors.
Learning outcomes:
Assessing radiographs relies on three criteria:
Health care often employs protocol-driven radiography, neglecting clinical history. This approach fulfills the first two criteria but disregards the treating physician's perspective, leading to debates, increased costs, resource wastage and reduced patient flow. Protocol-based practices ignore the evolving expertise of radiographers. We explore a solution: clinical history-based radiography, which aligns with clinical history and referrer's demands, addressing protocol limitations. In this workshop, we will discuss the why of the criteria discrepancy, and its potential impact on patients, society and government through case studies and the unique teaching approach of clinical history-based radiography employed at RMIT University.
Learning outcomes:
Join Dr Colin Dicks, Radiation Oncologist, author of Death, Dying & Donuts, and founder of Dying to Understand, a charity to promote death education. Being ‘death literate’ is an advantage for both professional and personal reasons. Understanding the end of life offers an opportunity to be better at life.
Learning outcomes:
This workshop introduces value-based health care and how health economics methodologies can be applied to the medical radiation professions. It will cover the foundations of health economic methods and the best scenarios for their use. Participants will be encouraged to think about value in their everyday work settings and how they can promote better value health care locally.
Learning outcomes:
This workshop will briefly introduce the concept of impostor phenomenon (aka impostor syndrome), discuss some of the ways it might manifest in different people and suggest various strategies to help individuals find ways to recognise and work with their own impostor voice.
Learning outcomes:
The Global Medical Radiation Practitioner Reference Group (GMRPRG) is a group of Australian radiographers and radiation therapists aiming to provide educational and technical assistance to our colleagues working clinically in Low- and Middle-Income Countries (LMICs). This workshop aims to develop a strategic plan helping to raise clinical practice standards in medical imaging and radiation therapy in developing nations, primarily in the Asia Pacific region. The strategic plan will be generated with initial presentations followed by breakout discussion groups contributing to a consensus-based plan.
Learning outcomes:



You can register for these sessions when you register for the conference. If you have already registered for the conference but would like to add either session, log back into your account and add the sponsored session for no cost.



